Frontotemporal Dementias
Shane S. Bush, Brian P. Yochim
Frontotemporal dementias (FTDs) are a group of heterogenous clinical syndromes marked by changes in behavior, personality, cognition, and mood. Clinical syndromes are characterized based on early signs and symptoms, including changes in behavior (behavioral variant FTD; bvFTD), language (nonfluent variant FTD, nfvFTD; semantic variant FTD, svFTD), and motor function (FTD-Motor Neuron Disease; Progressive Supranuclear Palsy, PSP; Corticobasal Syndrome; CBS), with significant overlap amongst syndromes. FTD typically presents at an earlier age of onset than other neurodegenerative disorders, most commonly between the ages of 45 and 64 years old. Progressive frontal and temporal lobe neurodegeneration drives symptom progression, with considerable variability based on the underlying protein pathology. Although FTD is typically sporadic, between 10% and 40% of cases are associated with an autosomal dominant pattern of genetic inheritance. There are no approved treatments that effectively target disease pathology; however, behavioral and environmental modifications, family and caregiver education and support, and symptom management can be effective.
Dementia
Current Perspectives in Research and Treatment
This book explores how our conception of dementia has changed since its initial discovery, taking in advancements in knowledge that translate into better ways to manage the condition.
Providing detailed reports of the latest research, the book explores the myriad forms of dementia. Written in accessible language, it looks at current methods of assessing and diagnosing the condition before turning to contemporary approaches to treatment. Chapters dedicated to often overlooked issues include raising awareness about how dementia affects the lives of those with an intellectual developmental disorder, the fundamental need to consider cultural differences, and the need to fully acknowledge and support informal carers. The final section of the text examines how COVID-19 has spotlighted serious gaps in healthcare for those living with dementia.
Frontotemporal dementia
David Ames, John T. O’Brien, Alistair Burns
Clinical understanding of frontotemporal dementia (FTD) has improved immensely over recent decades. For instance, the entry in the 1983 edition of the Oxford Textbook of Psychiatry for Pick’s Disease, one of the major pathologies underpinning FTD, stated, ‘ere are no specic clinical features to separate Pick’s disease from Alzheimer’s, and the distinction is generally made at autopsy not in life’. In contrast to what is now known, this statement could barely be further from the truth but highlights that if one applies the simplistic algorithm of noting progressive decline; falling below a cut-o on some global measure of cognition and excluding non-degenerative pathologies with a brain scan, then all degenerative dementias can seem similar.
Emotion, social functioning and activities of daily living in frontotemporal dementia
Howard J. Rosen, Robert W. Levenson
Social functioning in FTD is profoundly affected, and forms the basis for the clinical diagnosis of the behavioural variant of the disease (bv-FTD). In particular, there are deficits in emotional processing, but the inter-relationship of such deficits to other aspects of social functioning remains unclear. We studied patients with bv-FTD (n = 14) and AD (n = 14), and compared their performance on a test of emotion recognition with their scores on two carer-based assessments: the Disability Assessment for Dementia (DAD) of activities in daily living (ADL), and the Cambridge Behavioural Inventory (CBI). The bv-FTD group had significantly greater impairments in ADLs, and had higher scores on the CBI, compared to the AD group. Despite a deficit in emotion recognition, particularly involving negative emotions, in the FTD group relative to AD and controls, performance on this task did not correlate with ADL ratings which instead, correlated highly with carer-rated apathy levels on the CBI. The study highlights the multifactorial nature of social dysfunction in FTD which is important in the management of these patients and in designing effective behavioural and therapeutic interventions. The relationship of emotional processing to other aspects of social cognition in FTD is reviewed.
The experience of living with young onset dementia
Marjolein de Vugt, Janet Carter
Understanding Young Onset Dementia provides a state-of-the-art overview of approaches to care and evaluation for people with young onset dementia. It reviews the challenges in providing care and services, outlines new innovations in treatment and explores the impact of the condition to offer guidance about best practice in care.
‘They simply do not understand’: a focus group study exploring the lived experiences of family caregivers of people with frontotemporal dementia
Published in Aging & Mental Health
Jeroen Bruinsma, Kirsten Peetoom, Christian Bakker, Lizzy Boots, Frans Verhey, Marjolein de Vugt
Frontotemporal dementia (FTD) has a profound impact on the spouse and other family caregivers involved. While caregivers have a need for support, it is difficult for healthcare providers to respond to their specific needs. This qualitative study explores the lived experiences and needs of caregivers of persons with FTD to facilitate the development of support.
Behavioural variant Frontotemporal Dementia: Not all it seems?
Published in Neurocase
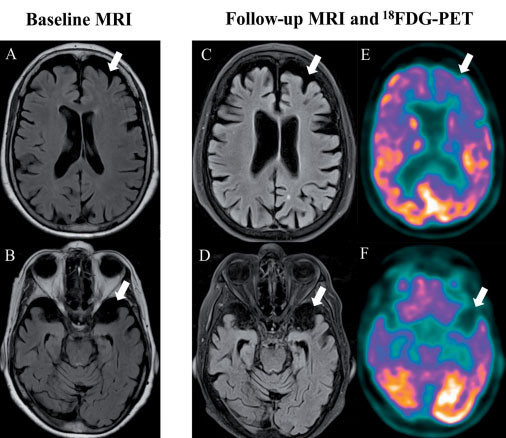
Background: The diagnosis of the behavioural variant of frontotemporal dementia (bvFTD) can be challenging. At present there is a paucity of prospective work addressing the specificity of current diagnostic criteria for bvFTD with respect to long-term outcome (i.e., false positives versus true positives).
Methods: Here we report two individuals who met current clinical criteria for bvFTD and who underwent detailed long-term clinical and neuropsychological follow-up. In addition, both had serial volumetric MRI and functional metabolic (FDG-PET) imaging separated by 5 years.
Metaphors for the Meaning of Caring for a Spouse with Dementia
Published in Journal of Multidisciplinary Healthcare
Spouses of people with young-onset frontotemporal dementia (YO-FTD) (age 65 years or younger) encounter special challenges. The diagnosis is scarcely known; the early onset is unexpected; and the disease is characterized by symptoms varying from those of other types of dementia. Caring implies increasing hardships, which can be difficult to communicate to others when applying for support. Metaphors create and communicate meaning and are increasingly used in health care and health interventions as ways to better understand the situation.
A peek at the window from the eye into the brain: potential use of OCT angiography in dementia
Published in Expert Review of Ophthalmology
Dementia is defined as the irreversible deterioration of acquired cognitive abilities (executive functions, memory, language, visuospatial, and motor) because of progressive neurodegeneration. According to a report by the World Health Organization (WHO) in 2018, dementia ranks as the 7th most common worldwide cause of death. In 2018, the globally estimated number of people afflicted by dementia was 50 million, a figure which is expected to triple by the year 2050 [Citation1]. The worldwide rapidly aging population and the resultant unprecedented rise in the incidence of dementia are anticipated to cause a greater burden in health expenditures both in underdeveloped and developed countries alike.
 China
China  Africa
Africa